(click graphic to open pdf link)
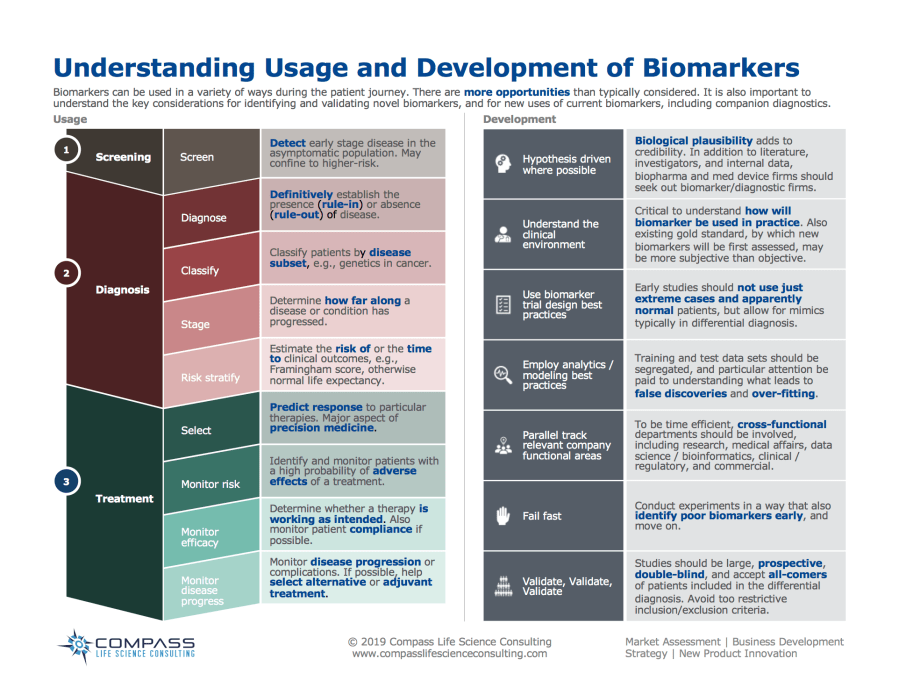
Biomarkers can used in a variety of ways during the patient journey. There are more opportunities than typically considered. It is also important to understand the key considerations for identifying and validating novel biomarkers, and for new uses of current biomarkers, including companion diagnostics.
Usage
SCREEN
Detect early stage disease in the asymptomatic population. May confine to higher-risk.
DIAGNOSE
Definitively establish the presence (rule-in) or absence (rule-out) of disease.
CLASSIFY
Classify patients by disease subset, e.g., genetics in cancer.
STAGE
Determine how far along a disease or condition has progressed.
RISK STRATIFY
Estimate the risk of or the time to clinical outcomes, e.g., Framingham score, otherwise normal life expectancy.
SELECT
Predict response to particular therapies. Major aspect of precision medicine.
MONITOR RISK
Identify and monitor patients with a high probability of adverse effects of a treatment.
MONITOR EFFICACY
Determine whether a therapy is working as intended. Also monitor patient compliance if possible.
MONITOR DISEASE PROGRESS
Monitor disease progression or complications. If possible, help select alternative or adjuvant treatment.
Development
Hypothesis driven where possible
Biological plausibility adds to credibility. In addition to literature, investigators, and internal data, biopharma and med device firms should seek out biomarker/diagnostic firms.
Understand the clinical environment
Critical to understand how will biomarker be used in practice. Also existing gold standard, by which new biomarkers will be first assessed, may be more subjective than objective.
Use biomarker trial design best practices
Early studies should not use just extreme cases and apparently normal patients, but allow for mimics typically in differential diagnosis.
Employ analytics / modeling best practices
Training and test data sets should be segregated, and particular attention be paid to understanding what leads to false discoveries and over-fitting.
Parallel track relevant company functional areas
To be time efficient, cross-functional departments should be involved, including research, medical affairs, data science / bioinformatics, clinical / regulatory, and commercial.
Fail fast
Conduct experiments in a way that also identify poor biomarkers early, and move on.
Validate, Validate, Validate
Studies should be large, prospective, double-blind, and accept all-comers of patients included in the differential diagnosis. Avoid too restrictive inclusion/exclusion criteria.
Start a conversation. Please provide contact information.

